Content
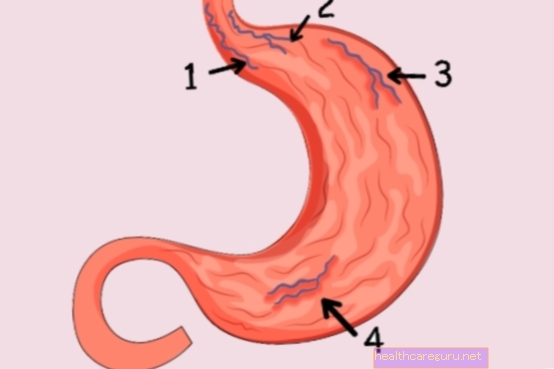
Varicose veins in the stomach are dilated and tortuous blood vessels that form on the wall of this organ, and they can be serious, because as they become larger, they are at risk of rupture and cause serious bleeding.
These varicose veins can form in the stomach due to increased resistance to blood flow in the portal vein, an important vein that drains blood from the abdominal organs, which can arise for several reasons, such as chronic hepatitis, liver cirrhosis, schistosomiasis or a thrombosis in the portal vein, for example. Better understand what is and what can cause portal hypertension.
Generally, gastric varices appear after or together with varicose veins in the esophagus, as well as in the rectum. The treatment for these varicose veins is indicated both to prevent and to stop bleeding, and can be done with beta-blocking drugs or surgical procedures, such as sclerotherapy, cyanoacrylate or elastic ligators, for example.
How to identify
Gastric varicose veins may not cause any symptoms, and can be identified in exams when portal hypertension is suspected, due to cirrhosis of the liver, for example. Esophageal varices are the most common, however, varicose veins in the stomach can form in 20% of cases, especially when the increase in pressure in the portal vein becomes more severe.
In addition, gastric varicose veins are less likely to rupture than esophageal varicose veins, however, they cause bleeding that is more severe and difficult to control. Some of the symptoms that indicate variceal bleeding are:
- Blackish stools with a foul smell;
- Vomiting with blood;
- Paleness, dizziness and palpitations.
Classification of types
The main tests to diagnose varicose veins are digestive endoscopy, doppler ultrasound and tomography. They can be in different locations in the stomach, being classified as:
Classification of gastric varices
- They are a continuation of esophageal varices, extending a few centimeters below the esophagogastric transition, through the small curvature of the stomach, the most common being;
- They are also an extension of esophageal varices, but towards the gastric fundus;
- These are isolated gastric varices, located at the bottom of the stomach;
- They are also isolated gastric varices, which can appear anywhere else in the stomach.
Gastric varicose veins are considered small when they measure less than 3 mm in diameter, medium when they are between 3 and 5 mm or large when they measure more than 5 mm in diameter. The larger the size of the varicose veins, the greater the risk of bleeding.
What causes gastric varices
Varicose veins in the stomach are formed by increased pressure in the portal vein, and the main reasons are:
- Chronic hepatitis;
- Hepatical cirrhosis;
- Schistosomiasis;
- Portal or splenic vein thrombosis;
- Budd-Chiari syndrome. Find out what this syndrome is like and how it happens;
- Malformations in the portal vein or in the inferior vena cava.
Varicose veins in the stomach can also be caused by a heart disease called constrictive pericarditis, in which fibrous tissue develops around the heart, and makes it difficult to function. Learn more about how it develops and the consequences of this disease.
How the treatment is done
If the varicose veins are small or if the doctor detects that there is a low risk of bleeding, there is no need for treatment of gastric varices, only their regular monitoring.
However, the doctor may, in some cases, recommend a treatment to prevent bleeding, especially if they measure more than 10 mm in diameter or there is a serious risk of bleeding, which can be done with beta-blocking drugs, which decrease strength blood flow, such as Propranolol, or the application of Cyanoacrylate, a kind of glue that eliminates the vessel.
When gastric varices present bleeding, treatment may include endoscopy for sclerotherapy, injection of cyanoacrylate or placement of elastic bandages, clips or springs, for example.
In addition to stopping the bleeding, as this is a serious situation, the doctor should take some precautions to protect the patient's life, such as replacing fluids with serum in the vein, making blood transfusions, if necessary, or using antibiotics to prevent abdominal infections. , common in patients with cirrhosis of the liver. Also check out other causes of stomach bleeding and what to do.