Content
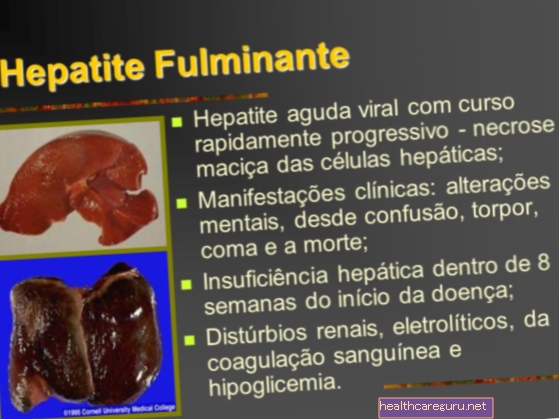
Fulminant hepatitis, also known as fulminant liver failure or severe acute hepatitis, corresponds to severe inflammation of the liver in people who have a normal liver or controlled liver disease in which the liver is no longer functional, which can result in death within a few days.
The symptoms of fulminant hepatitis are similar to those of other hepatitis, however the symptoms of this type of hepatitis can progress rapidly, with constantly dark urine, yellowish skin and eyes, low fever and general malaise. These symptoms progress quickly due to progressive liver involvement.
It is important that the diagnosis and treatment of fulminant hepatitis be made as soon as possible so that the symptoms can be controlled and there is no total loss of liver function, requiring the person to be hospitalized for treatment to be done.
Symptoms of fulminant hepatitis
The symptoms of fulminant hepatitis appear and evolve rapidly due to the constant involvement of the liver, which can leave the person very weak within a few hours. The main signs and symptoms of fulminant hepatitis are:
- Dark urine;
- Yellowed eyes and skin, a situation called jaundice;
- General malaise
- Low fever;
- Nausea and Vomiting;
- Pain in the right side of the abdomen;
- Abdominal swelling;
- Renal insufficiency;
- Hemorrhages.
When the person is very compromised, hepatic encephalopathy develops, which occurs when the inflammation reaches the brain, causing behavioral changes, sleep disturbances, disorientation, and even coma, being indicative of an advanced stage of the disease.
For the diagnosis of fulminant hepatitis, the doctor must observe the patient and request laboratory tests and a biopsy of the liver tissue that allows the severity of the lesions and sometimes the causes of the disease to be detected. See which tests assess the liver.
Main causes
Fulminant hepatitis usually occurs in people who have a normal liver, but it can also happen in people who have controlled liver changes, as in the case of hepatitis A and B, for example. Thus, in most cases, fulminant hepatitis is a consequence of other situations, the main ones being:
- Autoimmune diseases such as Reye's syndrome and Wilson's disease;
- Use of medication, most often as a result of self-medication;
- Consumption of teas for excess weight loss and without guidance;
- Lack of oxygen in the liver tissues;
- Excess fat in the liver during pregnancy.
When any of these situations is present, the person's liver can be severely affected, ceasing to be able to filter the blood to eliminate its impurities and to store vitamins and minerals, leading to the appearance of signs and symptoms of fulminant hepatitis.
When treatment is not started promptly, the liver stops converting ammonia into urea and the disease progresses affecting the brain, starting a condition called hepatic encephalopathy, which can be followed by failure or failure of other organs like kidneys or lungs, and possible coma.
How is the treatment
Treatment for fulminant hepatitis is done at the hospital and consists of using drugs to detoxify the liver. It is important that the person fast for a period and then receive an adequate, fat-free diet. Sometimes dialysis to purify the blood is necessary.
However, this is not always sufficient to cure fulminant hepatitis, as liver inflammation is often extensive and there is no chance of reversal. Thus, a liver transplant may be recommended so that it can be possible to achieve a cure. Understand how the liver transplant is done.
However, as fulminant hepatitis is a consequence of other changes, it is important that its cause is identified and treated, preventing further damage to the liver.