Content
The antibiogram, also known as Antimicrobial Sensitivity Test (TSA), is an exam that aims to determine the sensitivity and resistance profile of bacteria and fungi to antibiotics. Through the result of the antibiogram, the doctor can indicate which antibiotic is most suitable to treat the person's infection, thus avoiding the use of unnecessary antibiotics that do not fight the infection, in addition to preventing the emergence of resistance.
Normally the antibiogram is performed after the identification of microorganisms in large quantities in the blood, urine, feces and tissues. Thus, according to the identified microorganism and sensitivity profile, the doctor can indicate the most appropriate treatment.
How the antibiogram is made
To perform the antibiogram, the doctor will request the collection of biological material such as blood, urine, saliva, phlegm, feces or cells from the organ contaminated by microorganisms. These samples are then sent to a microbiology laboratory for analysis and cultivation in a culture medium that favors bacterial or fungal growth.
After growth, the microorganism is isolated and subjected to identification tests to reach the conclusion of the microorganism responsible for the infection. After isolation, the antibiogram is also performed so that the sensitivity and resistance profile of the identified microorganism is known, which can be done in two ways:
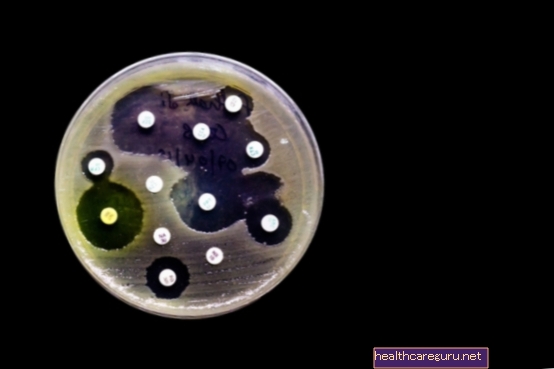
- Antibiogram by agar diffusion: in this procedure small paper discs containing different antibiotics are placed on a plate with appropriate culture medium for the growth of the infectious agent. After 1 to 2 days in the oven, you can see whether or not you hear growth around the disc. In the absence of growth, it is said that the microorganism is sensitive to that antibiotic, being considered the most suitable for the treatment of infection;
- Antibiogram based on dilution: in this procedure there is a container with several dilutions of antibiotic with different doses, where the microorganisms to be analyzed are placed, and the Minimum Inhibitory Concentration (CMI) of the antibiotic is determined. The container in which no microbial growth was observed corresponds to the dose of the antibiotic that must be used in the treatment, since it prevented the development of the microorganism.
Currently in the laboratories, the antibiogram is performed by equipment that tests resistance and sensitivity. The report released by the equipment informs which antibiotics the infectious agent was resistant to and which were effective in combating the microorganism and in what concentration.
Uroculture with antibiogram
Urinary tract infection is one of the most common infections in women, mainly, and in men. Therefore, it is common for physicians to request in addition to the type 1 urine test, the EAS, and the urine culture accompanied by an antibiogram. In this way, the doctor is able to check if there is any change in urine that is indicative of kidney problems, through EAS, and the presence of fungi or bacteria in the urinary tract that may indicate infection, through urine culture.
If the presence of bacteria in the urine is verified, the antibiogram is performed next so that the doctor can know which antibiotic is most suitable for treatment. However, in the case of urinary infections, antibiotic treatment is only recommended when the person has symptoms to prevent the development of microbial resistance.
Understand how urine culture is made.
How to interpret the result
The result of the antibiogram can take up to about 3 to 5 days and is obtained by analyzing the effect of antibiotics on the growth of microorganisms. The antibiotic that inhibits microbial growth is the one indicated to treat the infection, but if there is growth, it indicates that the microorganism in question is not sensitive to that antibiotic, that is, resistant.
The result of the antibiogram must be interpreted by the doctor, who observes the values of the Minimum Inhibitory Concentration, also called CMI or MIC, and / or the diameter of the inhibition halo, depending on the test that was performed. The IMC corresponds to the minimum concentration of antibiotic that is able to inhibit microbial growth and is in accordance with the standards of the Clinical and Laboratory Standards Institute, CLSI, and may vary depending on the antibiotic being tested and the microorganism that has been identified.
In the case of the agar diffusion antibiogram, where papers containing certain concentrations of antibiotics are placed in the culture medium with the microorganism, after incubation for about 18 hours it is possible to perceive the presence or not of inhibition halos. From the size of the diameter of the halos, it is possible to verify whether the microorganism is non-susceptible, susceptible, intermediate or resistant to the antibiotic.
The result must also be interpreted based on the determination of CLSI, which determines that for the susceptibility test of Escherichia coli to Ampicillin, for example, the inhibition halo less than or equal to 13 mm is an indication that the bacterium is resistant to the antibiotic and that a halo equal to or greater than 17 mm indicates that the bacterium is sensitive. Learn more about the result of urine culture with antibiogram.
Thus, according to the result of the antibiogram, the doctor can indicate the most effective antibiotic for fighting infection.
Why is it necessary to identify the correct antibiotic?
The use of antibiotics that are not suitable and effective for a microorganism delays the person's recovery, partially treats the infection and favors the development of microbial resistance mechanisms, making the infection more difficult to treat.
For this same reason, it is very important not to use antibiotics without the doctor's guidance and unnecessarily, as this may end up selecting microorganisms more resistant to antibiotics, reducing the options of drugs to fight infections.